Introduction
Tamoxifen has emerged as a fundamental drug in oncology, revolutionizing breast cancer treatment and management. Esteemed for both its efficacy and versatility, it has been a mainstay in medical treatments for decades. Additionally, Tamoxifen has shown effectiveness in a range of other medical conditions, reflecting its broad pharmacological utility.
What is Tamoxifen?
Tamoxifen is a medication that belongs to a class of drugs known as selective estrogen receptor modulators (SERMs). Chemically, it is a nonsteroidal compound with a complex molecular structure that allows it to interact selectively with estrogen receptors in various tissues. Its unique ability to either block or activate estrogen’s effects in different tissues classifies it as both an antagonist and an agonist, a duality that underpins its therapeutic applications.
The development of Tamoxifen can be traced back to the 1960s, with its initial use being in the treatment of infertility. However, its potential in breast cancer treatment soon became apparent, leading to its approval for this purpose in the 1970s. Since then, Tamoxifen has been a staple in hormone receptor-positive breast cancer treatment, both in adjuvant settings and for metastatic disease.
Mechanism of Action
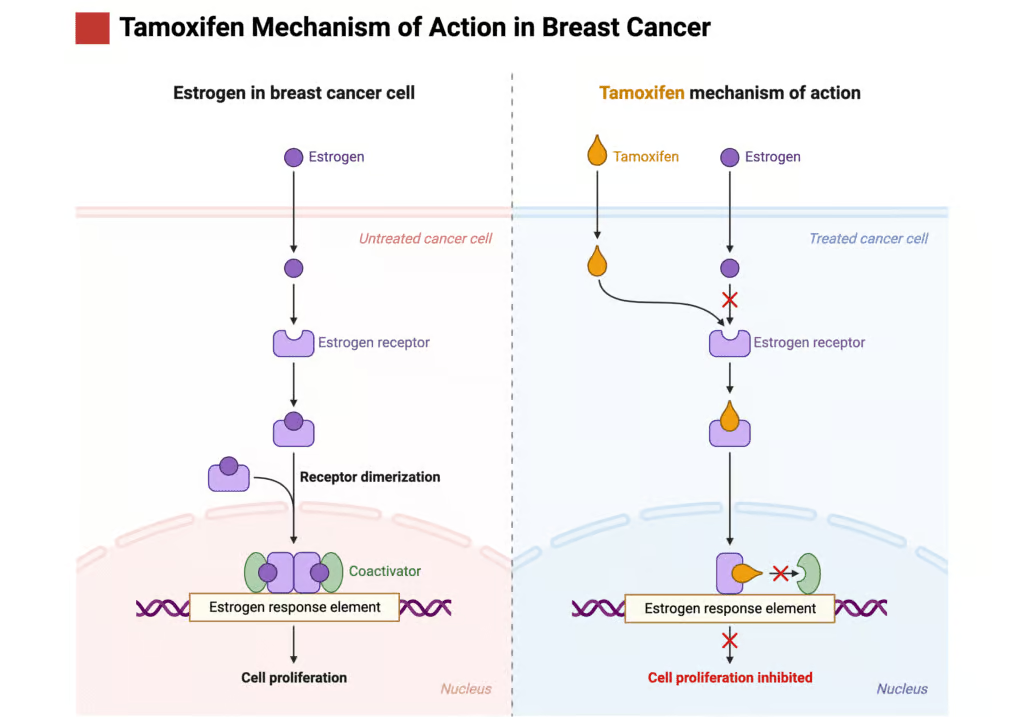
The pharmacological prowess of Tamoxifen lies in its intricate mechanism of action at the molecular level. As a selective estrogen receptor modulator (SERM), Tamoxifen exhibits a dualistic nature. It acts as an estrogen antagonist in breast tissue, effectively blocking estrogen receptors and thus inhibiting the proliferative action of estrogen on breast cancer cells. This blockade is crucial in treating and preventing estrogen receptor-positive breast cancers, where estrogen plays a key role in tumor growth.
Conversely, in other tissues like the bones and uterus, Tamoxifen acts as an estrogen agonist. This means it can mimic the action of estrogen, leading to beneficial effects such as the maintenance of bone density, which is especially advantageous in postmenopausal women. However, this agonistic action in the uterus also accounts for some of the drug’s side effects, like an increased risk of endometrial cancer.
Moreover, Tamoxifen’s influence extends beyond simple receptor blockade. Its metabolites, particularly endoxifen, are also potent anti-estrogens, contributing significantly to its overall therapeutic effect. The intricate interplay between Tamoxifen, its metabolites, and estrogen receptors across different tissues showcases the complexity and sophistication of its pharmacological action, underscoring its vital role in cancer therapeutics.
Uses of Tamoxifen
Treatment of Hormone Receptor-Positive Breast Cancer
Tamoxifen’s primary and most significant use is in the treatment of hormone receptor-positive breast cancer. In these cancer types, estrogen promotes tumor growth, and Tamoxifen, by blocking estrogen receptors, impedes this growth. It is used both in early-stage and advanced breast cancer and is particularly effective in premenopausal women.
Prevention of Breast Cancer
Tamoxifen also serves a preventive role, especially in high-risk individuals who have a family history of breast cancer or genetic predispositions. By blocking the potential effects of estrogen on breast tissue, Tamoxifen significantly reduces the risk of developing breast cancer in these high-risk groups.
Other Potential Uses
Besides its role in breast cancer, Tamoxifen has been explored for other uses. Notably, it was initially used in the treatment of infertility, particularly due to its ability to induce ovulation. Although less common today, this use highlights Tamoxifen’s diverse pharmacological effects.
Pharmacokinetics
Absorption
After oral administration, Tamoxifen is absorbed well from the gastrointestinal tract. However, its bioavailability is somewhat variable due to the effect of first-pass metabolism in the liver.
Distribution
In the body, Tamoxifen is extensively distributed in various tissues. It binds strongly to plasma proteins, such as albumin, which aids in its widespread distribution.
Metabolism
Tamoxifen’s metabolism is complex and primarily occurs in the liver. Cytochrome P450 enzymes (CYP2D6 being particularly significant) metabolize it into a number of metabolites, including the more potent endoxifen. These metabolites play a crucial role in its therapeutic efficacy.
Excretion
Tamoxifen and its metabolites are primarily excreted through feces, with a small amount also eliminated via urine. The elimination half-life of Tamoxifen is relatively long, contributing to its prolonged action in the body.
Clinical Efficacy
Efficacy in Clinical Trials
Numerous clinical trials and studies have underscored Tamoxifen’s efficacy in breast cancer treatment. These studies demonstrate significant improvements in survival rates, especially in early-stage hormone receptor-positive breast cancers. Tamoxifen has been shown to reduce the risk of cancer recurrence and is also effective in delaying the progression of metastatic breast cancer.
Comparison with Other Treatments
When compared with other breast cancer treatments, such as aromatase inhibitors, Tamoxifen remains a preferred choice, particularly in premenopausal women. Its unique mechanism of action and effectiveness in various stages of breast cancer make it a versatile and indispensable tool in breast cancer therapy.
Long-Term Outcomes
Long-term studies indicate that the benefits of Tamoxifen, particularly in preventing recurrence and increasing survival rates, persist even after the completion of the treatment course. However, the risk of certain side effects, such as endometrial cancer, necessitates careful monitoring during and after treatment.
Tamoxifen’s role in breast cancer treatment and prevention is well-established and backed by extensive clinical evidence. Its pharmacokinetics and varied uses underscore its importance in the pharmacological management of breast cancer, offering hope and improved outcomes for countless patients.
Side Effects
Common Side Effects
Tamoxifen therapy is often associated with various side effects, some of the common ones being:
- Hot flashes and night sweats, akin to menopausal symptoms.
- Vaginal discharge or dryness.
- Nausea and vomiting.
- Fatigue and mood swings.
These side effects are usually manageable and may diminish over time as the body adjusts to the medication.
Potential Long-Term Risks
More serious, but less common, long-term risks include:
- Endometrial Cancer: Tamoxifen’s estrogen-like effects on the uterine lining can increase the risk of endometrial cancer, especially in postmenopausal women.
- Thromboembolic Events: Such as deep vein thrombosis (DVT) and pulmonary embolism, due to its pro-thrombotic effects.
Regular monitoring and prompt reporting of symptoms are crucial in managing these risks.
Drug Interactions
Interactions with drugs like CYP2D6 inhibitors and anticoagulants can impact Tamoxifen’s effectiveness and safety. Managing such interactions is crucial, especially for patients receiving multiple medications.
- Patients with a history of deep vein thrombosis or pulmonary embolism due to the increased risk of recurrence.
- Those who are pregnant or planning to become pregnant, as it can harm the fetus.
- Patients with known hypersensitivity to Tamoxifen or any of its components.
Caution is advised in patients with liver impairment, as Tamoxifen is metabolized in the liver.
Dosage and Administration
Standard Dosing Guidelines
The standard dose of Tamoxifen for adults in the treatment of breast cancer is typically 20 mg per day, often taken as a single daily dose.
Adjustments for Specific Populations
- Renal Impairment: No significant adjustments are required, as Tamoxifen and its metabolites are primarily excreted in feces.
- Hepatic Impairment: Caution is advised, and dose adjustment may be necessary depending on the severity of impairment.
Administration Advice
- Tamoxifen can be taken with or without food.
- Consistency in taking the medication at the same time each day can help maintain steady blood levels.
- Patients should be advised not to double the dose in case of a missed dose.
In summary, while Tamoxifen is a critical medication in breast cancer treatment, understanding and managing its side effects, contraindications, drug interactions, and proper administration are key to optimizing its therapeutic effectiveness and ensuring patient safety.
Patient Education and Adherence
Importance of Patient Education
Educating patients about Tamoxifen is crucial for effective treatment management. Understanding the purpose, benefits, potential side effects, and the importance of adherence to therapy empowers patients to actively participate in their treatment and recognize when to seek medical advice.
Strategies to Improve Adherence
- Clear Communication: Thorough explanation of Tamoxifen’s role, dosage, and schedule.
- Managing Side Effects: Providing strategies to manage common side effects can reduce the likelihood of treatment discontinuation.
- Reminder Systems: Encouraging the use of medication reminders, like alarms or pill organizers.
- Regular Follow-ups: Scheduling regular appointments for monitoring therapy progress and addressing concerns.
- Support Networks: Encouraging participation in support groups for emotional and psychological support.
Conclusion
Recap of the Importance of Tamoxifen
Tamoxifen has undeniably been a game-changer in breast cancer therapy. Its ability to selectively modulate estrogen receptors has proven effective in treating and preventing hormone receptor-positive breast cancer. Beyond its primary application, Tamoxifen’s potential in other therapeutic areas has also been recognized, though its use in these areas is less common.
Future Prospects
The future of Tamoxifen in pharmacology looks toward enhancing its efficacy while minimizing side effects. Ongoing research includes:
- Improving Selectivity: Developing derivatives or alternative drugs with similar efficacy but fewer side effects.
- Personalized Medicine: Exploring genetic markers to predict patient response to Tamoxifen, aiming for more personalized and effective treatments.
- Combination Therapies: Investigating the efficacy of Tamoxifen in combination with other treatments to enhance outcomes.
Tamoxifen’s journey from an infertility treatment to a cornerstone in breast cancer therapy is a testament to the dynamic nature of pharmacological research and development. Its continued study not only contributes to our understanding of hormone receptor-positive breast cancer but also opens doors to potential new treatments and improvements in patient care. As research advances, Tamoxifen will likely continue to play a significant role, either in its current form or as a foundational model for new therapeutic developments.









