Introduction
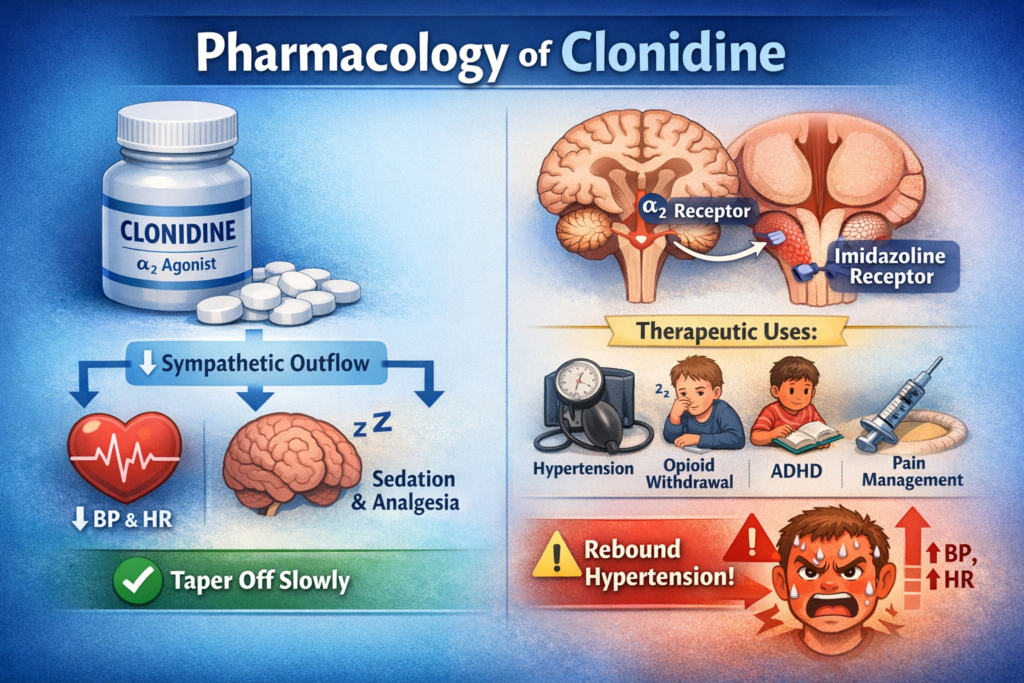
Clonidine is a centrally acting sympatholytic drug used mainly for its ability to reduce sympathetic outflow from the central nervous system. Pharmacologically, it is classified as an α₂-adrenergic receptor agonist with additional action at imidazoline receptors in the brainstem. Its major effect is a reduction in blood pressure and heart rate, but its sedative, analgesic, and autonomic-modulating properties also explain several of its clinical uses.
For MBBS students, clonidine is important because it links autonomic pharmacology with clinical medicine, especially in hypertension, withdrawal states, perioperative care, and certain neurologic or psychiatric indications.
Drug Class
Clonidine belongs to the group of central α₂ agonists, sometimes discussed under:
- centrally acting antihypertensive agents
- sympatholytic drugs
- α₂-adrenoceptor agonists
It is related pharmacologically to drugs such as methyldopa, guanfacine, and dexmedetomidine, though the degree of selectivity and clinical use differs.
Mechanism of Action
Primary mechanism
Clonidine stimulates presynaptic and postsynaptic α₂ receptors in the central nervous system, especially in the brainstem. The net effect is decreased sympathetic outflow from the vasomotor center. This leads to:
- reduced peripheral vascular resistance
- reduced heart rate
- reduced cardiac output
- fall in blood pressure
Imidazoline receptor action
Clonidine also acts on imidazoline receptors in the medulla, which further contributes to suppression of sympathetic tone and antihypertensive action.
Effect on norepinephrine release
By activating presynaptic α₂ receptors, clonidine inhibits release of norepinephrine from sympathetic nerve endings. That is why it is called a sympatholytic drug.
Spinal and analgesic actions
At the level of the spinal cord, α₂ receptor stimulation can inhibit transmission of pain signals, partly by reducing release of neurotransmitters such as substance P. This contributes to its analgesic and adjuvant anesthetic uses.
Hemodynamic Effects
The main cardiovascular effects of clonidine are:
- decrease in systolic and diastolic blood pressure
- bradycardia
- reduction in sympathetic-mediated vasoconstriction
An important point for exams: although clonidine lowers blood pressure mainly by central action, some α₂ agonists may produce a brief initial peripheral vasoconstrictor effect before the central hypotensive effect dominates. Clinically, the central effect is the important one.
Pharmacokinetics
Absorption
Clonidine is well absorbed orally. It is also available in transdermal form and in some settings as extended-release oral preparations.
Distribution
Because it is sufficiently lipid-soluble, clonidine crosses the blood-brain barrier, which is necessary for its central action.
Metabolism and excretion
A substantial proportion is eliminated by the kidney, and renal impairment may require caution or dose adjustment. This is clinically relevant because toxicity and exaggerated hypotension can occur more easily in susceptible patients.
Duration
Its action is long enough to permit regular oral dosing, while the transdermal system provides prolonged effect over days.
Pharmacological Actions
1. Cardiovascular system
This is the most important system for exam purposes.
Clonidine reduces:
- sympathetic tone
- blood pressure
- heart rate
Because sympathetic discharge is suppressed, it is useful in conditions where there is autonomic overactivity.
2. CNS effects
Clonidine produces:
- sedation
- calming effect
- reduced arousal
- sometimes fatigue or drowsiness
These effects are directly related to its central action and explain both its therapeutic uses and adverse effects. Drowsiness is one of the commonest adverse reactions.
3. Analgesic action
Clonidine has antinociceptive properties, particularly when used as an adjuvant in anesthesia or pain management. It enhances descending inhibitory pain pathways and reduces neurotransmitter release in the dorsal horn.
4. Autonomic stabilization
Because it suppresses sympathetic hyperactivity, clonidine can reduce symptoms such as:
- tachycardia
- sweating
- tremor
- restlessness associated with withdrawal states
This is why it is used in opioid withdrawal and sometimes other withdrawal syndromes.
Therapeutic Uses
1. Hypertension
Historically, clonidine was used more commonly in hypertension. It is effective but not usually a first-line drug now because of:
- sedation
- dry mouth
- rebound hypertension on sudden withdrawal
Still, it remains useful in selected patients, especially where central sympatholysis is beneficial. DailyMed lists clonidine as indicated for treatment of hypertension.
2. Hypertensive urgency / resistant hypertension
In some settings, clonidine may be used to lower blood pressure relatively quickly, though use varies by guideline and clinical setting.
3. ADHD
Extended-release clonidine is approved in some settings for attention-deficit/hyperactivity disorder, especially in children, often as monotherapy or adjunctive therapy.
4. Withdrawal syndromes
Clonidine is useful in opioid withdrawal because it relieves autonomic symptoms such as:
- sweating
- tachycardia
- hypertension
- anxiety
- restlessness
Important exam point: it does not treat craving as effectively as opioid substitution therapies, but it reduces sympathetic symptoms.
5. Perioperative and anesthetic use
Clonidine may be used as:
- preanesthetic medication
- adjuvant to regional anesthesia
- adjunct in pain management
- sedative in critical care settings
Its benefits include sedation, reduction of anesthetic requirement, and some analgesic-sparing effect.
6. Neuropathic pain / cancer pain adjunct
It may be used as an adjunct in difficult pain states, especially in specialized settings. StatPearls notes an approved adjunctive role in severe cancer-related pain.
7. Tourette syndrome / tics
Clonidine may help control tics in some patients.
Adverse Effects
The adverse effects of clonidine are very important in exams because they directly reflect its mechanism.
Common adverse effects
- dry mouth
- drowsiness / sedation
- dizziness
- constipation
- fatigue
- bradycardia
- hypotension
DailyMed specifically notes that common adverse effects are dose-related, with dry mouth and drowsiness among the most frequent.
Important adverse effects
- marked bradycardia
- postural hypotension
- depression or mental dullness in some patients
- decreased alertness
- sexual dysfunction in some cases
- skin reactions with transdermal patches
Toxicity / overdose
Overdose may produce:
- hypotension or sometimes early hypertension
- severe bradycardia
- CNS depression
- respiratory depression
- miosis
- hypothermia
- coma in severe poisoning
Rebound Hypertension: A Classic Viva Question
One of the most important features of clonidine is rebound hypertension after abrupt withdrawal.
Why does it happen?
During chronic clonidine therapy, sympathetic tone is suppressed. Sudden stoppage causes a surge in sympathetic activity, producing:
- severe rise in blood pressure
- tachycardia
- headache
- nervousness
- sweating
- agitation
Clinical significance
This can be dangerous and may lead to hypertensive encephalopathy or cerebrovascular complications.
Exam rule
Never stop clonidine abruptly. Taper it gradually.
A particularly important caution is the patient also taking a beta-blocker, because the withdrawal reaction can be worse.
Contraindications and Precautions
Use clonidine cautiously in:
- bradycardia
- hypotension
- severe cardiovascular disease
- cerebrovascular disease
- renal impairment
- elderly patients
- patients who may not adhere reliably, because missed doses can precipitate rebound hypertension
It should also be used carefully with other CNS depressants because sedation may be enhanced.
Drug Interactions
Important interactions include:
1. CNS depressants
Alcohol, sedatives, and other CNS depressants may increase:
- sedation
- dizziness
- psychomotor impairment
2. Other antihypertensive drugs
May cause additive hypotension.
3. Beta-blockers
A very important exam interaction. If clonidine is withdrawn abruptly while the patient remains on a beta-blocker, rebound hypertension may become more severe.
4. Drugs affecting heart rate
Concomitant drugs that lower heart rate may increase the risk of bradycardia.
5. Tricyclic antidepressants
These may reduce the antihypertensive effect of clonidine by interfering with central adrenergic pathways. This is a classic pharmacology teaching point.
Comparison with Methyldopa
This is useful for short notes.
Clonidine
- α₂ agonist
- reduces sympathetic outflow
- sedation and dry mouth are common
- rebound hypertension on abrupt withdrawal is characteristic
- used in hypertension, withdrawal states, ADHD, perioperative settings
Methyldopa
- converted to α-methylnorepinephrine in CNS
- also reduces sympathetic outflow
- especially known for use in hypertension in pregnancy
- adverse effect profile includes hemolytic anemia and hepatitis, which are not typical of clonidine
Comparison with Dexmedetomidine
- Both are α₂ agonists
- clonidine is less selective than dexmedetomidine
- dexmedetomidine is used more in ICU and procedural sedation
- clonidine is more familiar as an antihypertensive and autonomic-modulating drug
Clinical Pearls for MBBS Students
- Clonidine is a central α₂ agonist.
- It lowers blood pressure by decreasing sympathetic outflow.
- Common adverse effects are dry mouth, sedation, dizziness, constipation, bradycardia.
- It is used not only in hypertension, but also in withdrawal syndromes, ADHD, pain, and perioperative medicine.
- Abrupt withdrawal causes rebound hypertension — this is one of the highest-yield points.
Short Exam-Style Summary
Clonidine is a centrally acting α₂-adrenergic agonist and imidazoline receptor agonist that reduces sympathetic outflow from the CNS. It lowers blood pressure and heart rate, and also produces sedation and analgesic effects. It is used in hypertension, opioid withdrawal, ADHD, and as an adjunct in anesthesia/pain management. Important adverse effects include dry mouth, drowsiness, constipation, bradycardia, and hypotension. Abrupt discontinuation may cause rebound hypertension, so the drug must be tapered gradually.
One-Minute Revision Box
Think of clonidine as:
“Central α₂ agonist → ↓ sympathetic outflow → ↓ BP, ↓ HR, sedation, dry mouth, rebound HTN on withdrawal.”
A good memory line:
Clonidine calms the sympathetic system, but stopping it suddenly causes the system to rebound violently.
Quick self-check
Try answering these without looking back:
Why is clonidine relevant in opioid withdrawal?
What receptor action explains clonidine’s antihypertensive effect?
Why does clonidine cause sedation?
What is the most important danger of abrupt withdrawal?
Name two non-hypertension uses of clonidine.
Medical Disclaimer
The medical information on this post is for general educational purposes only and is provided by Pharmacology Mentor. While we strive to keep content current and accurate, Pharmacology Mentor makes no representations or warranties, express or implied, regarding the completeness, accuracy, reliability, suitability, or availability of the post, the website, or any information, products, services, or related graphics for any purpose. This content is not a substitute for professional medical advice, diagnosis, or treatment; always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition and never disregard or delay seeking professional advice because of something you have read here. Reliance on any information provided is solely at your own risk.
Community Notes
Join the Discussion
Ask follow-up questions, add clinical perspective, or share a useful clarification for the next reader.